More patients across England are paying for private healthcare as NHS waiting times remain stubbornly high. New research from Healthwatch England shows a sharp rise in people bypassing NHS waiting lists for faster diagnosis, consultations and surgery. The shift highlights growing concern about delayed treatment, diagnostic backlogs and limited hospital capacity. As patients search for quicker access to care, private healthcare is increasingly seen as a practical alternative to long NHS waiting times.
The number of patients paying for private healthcare in England has risen sharply in recent years, according to new figures from Healthwatch England. The patient watchdog reports that the proportion of people funding their own care has increased significantly over the past two years, highlighting the growing pressure on NHS services and the widening gap between demand for treatment and the system’s capacity to deliver it.
In 2023, around 9 per cent of people surveyed said they had used private healthcare within the previous year. By the end of 2025 that figure had risen to 16 per cent. The data comes from two nationally representative surveys, with 1,758 respondents in September 2023 and 2,593 adults surveyed across England at the end of last year.
The most striking finding is not simply that more people are turning to private care, but why they are doing so. Nearly four in ten respondents who paid for treatment privately said they did so because NHS waiting times were too long. Another 30 per cent cited convenience as the main reason for going outside the public system.
These figures reflect a shift that has been building for several years. For many patients the decision to seek private treatment is not ideological. It is practical. When a diagnostic test, specialist consultation or surgical procedure carries a waiting time measured in months rather than weeks, patients who can afford to do so increasingly look for alternatives.
Healthwatch England warned that this trend risks reinforcing the emergence of a two-tier healthcare system. Those who can pay avoid the wait. Those who cannot remain on it.
Income differences already appear to influence who accesses private care. Respondents earning more than £80,000 a year were significantly more likely to say they had paid for private healthcare in the past year. That disparity underlines the broader structural concern: when waiting times lengthen, healthcare access begins to correlate with income rather than clinical need.
The backdrop to these findings is the ongoing NHS waiting list challenge. While recent figures show modest improvement, the scale of the backlog remains enormous. At the end of January 2026 there were approximately 7.25 million treatments waiting to be carried out in England. That represents a slight decline from 7.29 million the previous month and marks the third consecutive monthly fall, bringing the list to its lowest level since early 2023.
Even so, the numbers remain historically high. Diagnostic services illustrate the pressure clearly. The number of patients waiting for tests such as scans and investigations has risen sharply since 2020, reaching close to 1.8 million in early 2026.
Mapped: The tens of thousands waiting for hip and knee ops
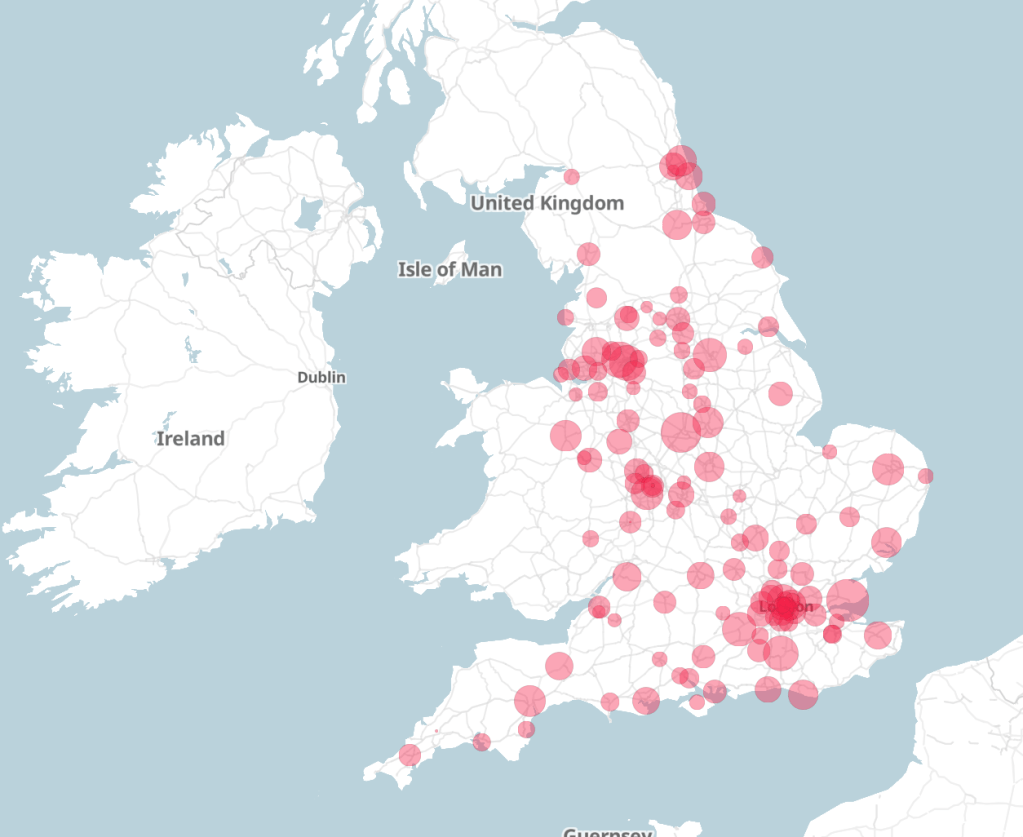
For patients facing uncertainty about diagnosis or treatment timelines, these statistics translate into lived reality. Waiting lists are not abstract policy metrics. They are months of unresolved symptoms, delayed reassurance or postponed intervention.
Chris McCann, acting chief executive of Healthwatch England, acknowledged the efforts being made to address elective care backlogs through the NHS 10-Year Plan but warned that progress must accelerate if public confidence is to recover. Patients waiting for hospital care should receive consistent communication and updates about their referral status, he said, along with clear guidance on managing symptoms during the waiting period.
Administrative clarity is particularly important. Patients often report uncertainty about whether their referral has been received, accepted or scheduled. Regular updates confirming that they remain on the waiting list, together with advance notice of cancellations or rescheduling, would reduce anxiety and improve transparency.
From the perspective of the independent sector, the increase in privately funded care reflects what industry leaders describe as a structural shift in patient behaviour. David Hare, chief executive of the Independent Healthcare Providers Network, said it is unsurprising that people are increasingly willing to pay for treatment themselves or access private medical insurance through their employer.
Patients prioritise their health and the health of their families above almost everything else. When timely care is unavailable within the public system, the private sector becomes the practical alternative. This applies across a broad range of services including general practice appointments, diagnostic testing, specialist consultations and surgical procedures.
In effect, private healthcare is becoming part of the routine pathway for many patients rather than an exceptional option.
Government officials maintain that the NHS is making progress. NHS England reports that 2025 saw record numbers of appointments, tests and scans delivered across the system, contributing to the gradual reduction in waiting lists. General practice teams are now delivering more than one million appointments every working day, while initiatives such as Pharmacy First aim to redirect certain conditions away from GP surgeries and improve access to care.
The Department of Health and Social Care has also stated that it intends to eliminate what it describes as the unacceptable two-tier healthcare system inherited by the current government.
Yet the data suggests that for many patients the two-tier reality is already emerging. When nearly one in six people report paying privately for care, the shift is no longer marginal. It is systemic.
For healthcare platforms such as My Medical Gateway the trend is not surprising. The demand for faster diagnosis, transparent pricing and predictable access to treatment continues to grow across Europe. Patients increasingly view healthcare access through the same lens they apply to other services: speed, clarity and choice matter.
As waiting lists remain elevated and patient expectations evolve, the boundary between public provision and privately accessed care will continue to shift. The central policy question is not whether private healthcare will play a role. It already does. The question is how systems adapt to ensure that access to timely treatment does not become determined primarily by the ability to pay.


Leave a comment